#InThisTogether: 03 AUG 2020
 With everything going on during the COVID-19 crisis, we wanted to share some of the stories about what Cook people are doing during this difficult time. All around the Cook world, we are #InThisTogether, and we would love to hear stories about how you and your coworkers are stepping up to make a difference. If you have a story to share, please email us at BlogEditor@CookMedical.com.
With everything going on during the COVID-19 crisis, we wanted to share some of the stories about what Cook people are doing during this difficult time. All around the Cook world, we are #InThisTogether, and we would love to hear stories about how you and your coworkers are stepping up to make a difference. If you have a story to share, please email us at BlogEditor@CookMedical.com.
—
During pandemic times
Written by Terrie Nicodemus, a Written Content specialist in Corporate Marketing and Communications
On a normal basis
After nine years of working at Cook as a senior clinical specialist for the Vascular division, based in the UK, Heather Garnett faced some of the most bizarre months in her entire career in 2020.
In her role, Heather supports customers with Cook’s portfolio of aortic devices, predominantly the customized medical devices serving complex aortic disease. From the moment a physician contacts her to review scans and discuss the patient’s options, Heather’s expertise is relied upon by physicians as she helps them to consider what’s best for the patient.
Heather is also often in the operating room (OR) with the physician’s team as they implant customized devices. She is there to provide product and clinical support during the case.
“They could have questions about proper positioning of the device for example, and I’m right there in the surgery room to talk through any that they might have.”
“The most bizarre months ever”
But the in-person physician meetings, hospital visits, and operating room support Heather did on an almost daily basis for nine years came to an abrupt halt on March 19 due to the UK hospitals’ response to the COVID-19 pandemic.
“The country-wide lockdown was announced on my 40th birthday,” recalled Heather. “It wasn’t quite the party I planned.” The next eight weeks were what she called, “the most bizarre months ever.”
Heather had literally no cases for five weeks. Many hospitals were not allowing visits from companies unless there was a specific clinical reason. Going from being out every day to suddenly working from home was a difficult transition.
“I have two small children at home, so merging home and work together was challenging. My job is not just a 9-to-5 job. I would get calls day and night. It is a big part of my life. I missed my customers and teammates dreadfully,” she explained.
During that five-week period, Heather spent her time catching up on case reviews and keeping in touch with customers remotely. The divisional support and Cook training teams developed online trainings to help home-based employees make productive use of their time.
The majority of Heather’s work is in the northern part of the UK, which did not have as many COVID-19 cases as southern UK. Hospitals in the north began reopening for elective procedures earlier than other parts of the country. Heather witnessed a slow start-up of elective procedures in mid-May.
“Work is changing for me. I continue to get busier and slowly back to normal, but for others it’s still the same. Many of the procedures have been put on hold, but patients are still out there and in need of treatment,” she said.
Supporting cases through the pandemic
Hospital procedures in the UK and Ireland were changing in the new pandemic environment. Heather began to be anxious about what she would be facing going into the hospitals again for an elective case.
“I wasn’t sure what to expect on my return and felt a little uneasy on my first case back. Once I was there, it was quite reassuring being with the hospital staff, and once in the OR it was business as usual to get the case done.” said Heather. “I am very conscious that I’m going into a department that is under stress, and I make sure to follow all of their guidelines.”
Procedures are normalizing with a new normal, and it has become increasingly important for her to become familiar with local guidelines. Each province is handling safeguards in a slightly different way. Heather’s new routine is to prepare ahead of time by emailing her customers to determine specific guidelines she needs to follow.
At one hospital, immediately after the lockdown eased, she was required to provide a formal email from the physician confirming she was required in the OR for a specific clinical reason. Cook Medical also provided a formal letter confirming she was “a key worker” and required to travel. She noticed small changes like increased hand hygiene requirements, restrictions at certain points in the hospital where a mask and scrubs were required, and physical distancing rules. Some hospitals mandate visors to be worn, and most facilities require all staff to leave the OR for a specified amount of time when a patient is intubated. However, all patients across all provinces must self-isolate for two weeks before an elective procedure. The patients are tested for COVID before their elective procedure. The test results must be negative before they can have the procedure.
Navigating NHS and private hospitals
As the number of COVID cases rose during the height of the pandemic in the UK, some National Health Service (NHS) hospitals had agreements with private hospitals to treat patients with elective cases. Many of the private hospitals in the UK have not been involved in the treatment of COVID patients, said Heather. The NHS is the UK’s main healthcare system and is publicly funded and supported by taxpayers. The UK has two main types of hospitals, NHS hospitals and private, insurance-based hospitals. During the pandemic, Heather has carried out some elective cases at private hospitals.
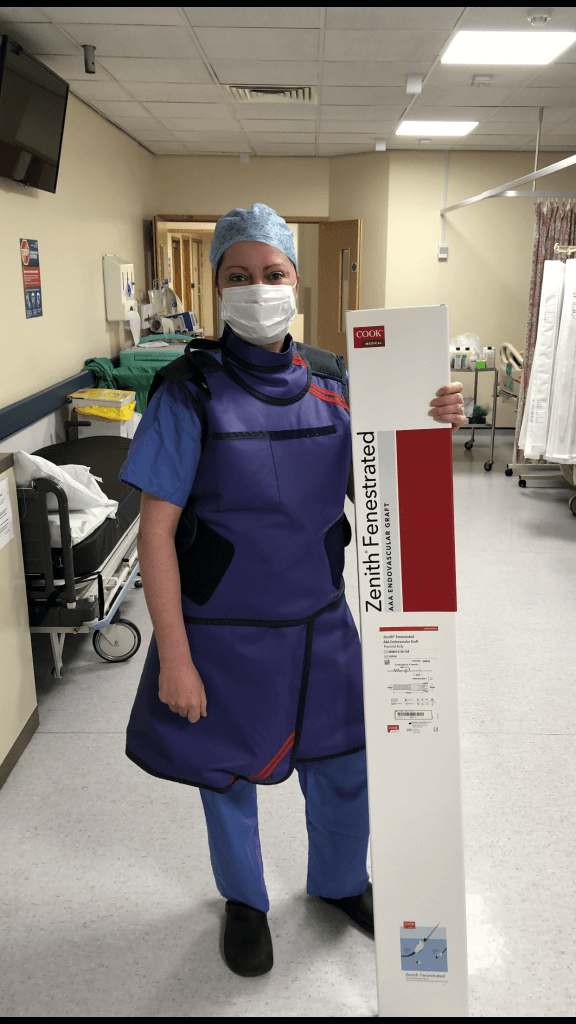
“That involves quite a bit of additional work for me,” she said. “The private hospitals are much smaller than NHS hospitals and aren’t used to performing complex aortic procedures.”
While working within private hospitals, Heather is busy making sure the product kit is available at these facilities, ensuring any additional accessory kits are also available, and confirming the staff has everything they need on site to complete the case.
“At one point, I was carrying 15 stent boxes from a private hospital back to an NHS hospital. Those boxes are almost as big as me!” she said.
Thoughts on the future
With Heather’s unique view of the UK hospital system, working in the trenches with physicians and staff, she maintains a positive outlook. She predicts her role will be getting back to normal slowly and meetings at hospitals will continue to be restricted in the immediate future, but that product presentations in that setting won’t be happening until later in the year in the UK.
“The stresses and strains of this pandemic will affect hospital systems for a long time, but they have found ways to adapt and prepare themselves. I’m pleased to be getting back to my cases and I find that the staff are just as happy to see me as I am to see them,” she said.
—
Want to read more stories like this?
Click the images below to check out other Life@Cook blog posts.

Great work Heather!!
You’re a super star Heather
Well done Heather
Thanks for sharing your inspiring story… You’re AWESOME Heather!
Thank you Heather and to your team! Proud of you. Keep well.
Excellent blog Heather, well done!
Great work Heather, well done during these difficult times.
It must have been difficult especially juggling with two young children.
Stay safe and take care
Strong work Heather. Great to hear Access is opening back up.
Great work, Heather. Thanks for sharing your story and for continuing to help our customers in these challenging times!
Great….I appreciate your dedication to serving patients. Really this pandemic teaches us so many good things too for example ” How to work in challenging situation.”
Nice one Heather.
Fabulous work Heather and great blog.
Heather thank you for sharing your story!!